Mastering Clinical Trial Timelines & Milestones Management
Clinical trial timelines fail quietly before they fail visibly. The missed milestone usually begins weeks earlier with a late contract, unclear site dependency, unresolved protocol question, slow IRB package, weak enrollment math, or monitoring backlog nobody escalated soon enough. Strong timeline management connects clinical trial project planning, clinical trial protocol management, risk management in clinical trials, and effective stakeholder communication into one disciplined operating rhythm that protects study quality, cost, enrollment, and inspection readiness.
1. Why Clinical Trial Timeline Management Is a Risk-Control Skill
A clinical trial timeline is not a calendar decoration. It is the operational proof that the protocol can move through start-up, activation, recruitment, treatment, monitoring, data cleaning, database lock, reporting, and closeout without losing control of quality. A weak timeline hides dependencies; a strong timeline exposes them early. That is why timeline ownership must sit close to clinical trial sponsor responsibilities, vendor management in clinical trials, clinical trial resource allocation, and clinical trial budget oversight.
The first mistake is building a timeline from target dates instead of study reality. A target date says when the sponsor wants the first site activated. A real timeline asks whether the protocol is final, the ICF is approved, the investigator brochure is current, the EDC build is ready, the lab manual is complete, contracts are moving, regulatory documents are collected, and the site has trained staff. Those details connect directly to informed consent procedures, clinical trial documentation under GCP, managing regulatory documents, and essential GCP training requirements.
The second mistake is tracking milestones after they slip. Effective milestone management is forward-looking. It uses leading indicators: overdue document collection, site contract cycle time, IRB submission aging, screen failure rate, query backlog, monitoring follow-up aging, vendor deliverable delays, and enrollment velocity against forecast. A study team that waits for the milestone date to pass has already lost time. Strong teams use clinical trial monitoring techniques, site selection and qualification, clinical data management systems, and EDC system planning to see risk before it becomes delay.
| Milestone Area | What Must Be Tracked | Common Delay Signal | Best Management Action |
|---|---|---|---|
| Protocol finalization | Final protocol, synopsis alignment, schedule of activities, endpoint definitions | Teams plan start-up while major protocol questions remain open | Resolve design dependencies using protocol development fundamentals |
| Budget planning | Site costs, vendor costs, monitoring costs, pass-throughs, screen failure assumptions | Timeline pressure appears because the budget never matched study complexity | Compare assumptions against clinical trial cost planning |
| Vendor selection | CRO, labs, imaging, EDC, ePRO, drug supply, translation, logistics | Vendors are selected after critical deliverables are already due | Build vendor dates into vendor management controls |
| Site feasibility | Patient population, competing trials, staff capacity, equipment, prior performance | Sites overpromise enrollment without evidence | Use documented feasibility tied to site qualification practices |
| Site selection | Selection criteria, activation readiness, investigator experience, patient access | High-prestige site slows the trial due to poor operational readiness | Score sites against startup speed and enrollment proof |
| Regulatory package | CVs, licenses, financial disclosure, training records, delegation documentation | One missing document blocks submission | Track each artifact under regulatory document management |
| IRB submission | Submission packet, consent form, recruitment materials, safety documents | Submission clock starts late because packet ownership is unclear | Assign owners using IRB responsibility guidance |
| Contract execution | CTA review, legal redlines, budget negotiation, payment terms | Legal negotiation silently becomes the critical path | Escalate aged redlines during weekly governance review |
| Informed consent approval | Correct version, language needs, local requirements, re-consent plan | Sites train on one version and receive approval for another | Version-control consent using informed consent essentials |
| EDC build | CRFs, edit checks, visit schedule, user access, testing, data standards | EDC goes live after first patient workflow has already started | Plan CRF design through CRF best practices |
| Randomization setup | IRT/IWRS readiness, randomization list, stratification, emergency unblinding | Activation is delayed because randomization workflow was tested late | Validate against randomization requirements |
| Blinding controls | Unblinded roles, pharmacy process, accountability, emergency procedures | Site activation happens before blinding responsibilities are understood | Train teams using blinding principles |
| Lab readiness | Lab manuals, kits, sample labels, shipping routes, normal ranges, portal access | First patient visit occurs before kit logistics are stable | Confirm kit and shipping readiness before activation |
| Drug supply | Release, labeling, import, depot, site shipment, temperature monitoring | Site is activated but study drug cannot be dispensed | Manage supply as a critical-path dependency |
| Site initiation visit | Training, delegation, protocol walkthrough, systems access, issue escalation | SIV completed while staff still lack system access | Align training with GCP compliance strategies |
| First site activated | Greenlight checklist, approvals, contracts, supply, systems, staff training | Activation is declared before the site can actually screen | Use activation criteria that require operational readiness |
| First patient screened | Recruitment source, prescreening quality, consent timing, screening procedures | Screening starts late because recruitment planning was theoretical | Connect planning to patient recruitment strategy |
| First patient randomized | Eligibility verification, randomization access, drug assignment, baseline completeness | Randomization is delayed by missing eligibility evidence | Pre-check criteria with protocol deviation prevention |
| Enrollment velocity | Screened, failed, randomized, pending, withdrawn, site-level rate | Aggregate enrollment hides poor-performing sites | Track site-level velocity and screen failure reasons weekly |
| Monitoring schedule | Visit cadence, remote review, SDV/SDR scope, follow-up letters | Monitoring backlog grows while enrollment accelerates | Adjust cadence using CRA monitoring techniques |
| Protocol deviations | Deviation log, root cause, CAPA, repeat issues, preventability | Deviation review happens after patterns become entrenched | Trend deviations through GCP deviation controls |
| Adverse event reporting | AE capture, SAE escalation, follow-up, reconciliation, medical review | Safety reconciliation is delayed until database cleaning | Track safety timelines with AE management practices |
| Query management | Open queries, aging, repeat data issues, site response quality | Database lock slips because data cleaning started too late | Control query aging through weekly site-level review |
| Interim analysis | Data cut, clean data scope, DMC package, unblinding protections | Data cut is planned before endpoint data is clean | Coordinate with DMC responsibilities |
| Last patient in | Enrollment closure, site communication, remaining screening pipeline | Study closes enrollment while qualified subjects are still in screening | Use a controlled LPI decision process |
| Last patient last visit | Visit completion, missed assessments, final safety follow-up, withdrawals | LPLV is declared with unresolved final visit data gaps | Verify visit completion against protocol schedule |
| Database lock | Query closure, coding, reconciliation, external data, PI sign-off | Lock date slips because external vendors submit late data | Run lock readiness meetings before LPLV |
| Clinical study report | Tables, listings, figures, narratives, safety summaries, protocol deviations | CSR writing starts before analysis decisions are finalized | Coordinate with medical writing workflows |
| Site closeout | Essential documents, drug accountability, final payments, archiving, open issues | Closeout is delayed by unresolved monitoring findings | Prepare closeout using inspection readiness standards |
| TMF completeness | Filing timeliness, missing artifacts, QC findings, final reconciliation | TMF cleanup becomes a rescue project near closeout | Track TMF health throughout the study |
| Final archiving | Retention requirements, access control, final transfer, long-term availability | Teams lose evidence after study team turnover | Archive according to GCP documentation principles |
2. Build the Timeline From the Protocol, Not From Optimism
The protocol is the real timeline engine. Every visit, procedure, endpoint, lab draw, imaging requirement, washout period, safety follow-up, randomization step, and assessment window creates work. A timeline built without protocol mapping becomes a fantasy schedule. A stronger team converts the schedule of activities into operational tasks, then links each task to owner, predecessor, approval requirement, system dependency, site burden, and risk level. This is why clinical trial protocol guidance, primary and secondary endpoints, placebo-controlled trial design, and clinical trial sample size planning matter before dates are assigned.
Timeline planning should begin with milestone categories: study design, vendor readiness, country start-up, site activation, enrollment, treatment, monitoring, data cleaning, analysis, reporting, closeout, and archiving. Each category should have a critical-path owner. If nobody owns the path between final protocol and first patient in, the team discovers too late that IRB approval, contract execution, EDC readiness, study drug shipment, and staff delegation were never synchronized. Proper planning connects clinical research project planning, top clinical trial PM terms, clinical trial technology innovations, and clinical trial templates and SOPs.
The enrollment forecast deserves special scrutiny because many timelines collapse through wishful recruitment math. Site teams may estimate based on patient population size while ignoring competing trials, inclusion criteria burden, travel demands, visit frequency, lab requirements, screen failure probability, and consent hesitancy. A better forecast separates prescreened, screened, screen failed, randomized, withdrawn, and completed subjects by site. That discipline is closely linked to CRC patient recruitment, clinical trial volunteer registries, clinical trial patient education resources, and virtual clinical trial planning.
The most professional timelines include buffers, but buffers should be placed intelligently. Add time around high-uncertainty dependencies: contract negotiation, import permits, central lab setup, imaging vendor readiness, translations, recruitment ramp-up, data transfer testing, and interim analysis preparation. Avoid hiding delay inside vague “contingency” blocks. Sponsors, CROs, CRAs, CRCs, and vendors need to see where uncertainty lives so they can manage it. This level of control reinforces risk management in clinical trials, clinical trial resource allocation, sponsor responsibilities, and stakeholder communication strategies.
3. Manage Milestones Across Start-Up, Enrollment, Monitoring, Data, and Closeout
Study start-up is the milestone zone where operational discipline pays off fastest. The team should track site feasibility completion, essential document collection, CTA status, budget negotiation, IRB submission, consent approval, system access, staff training, supply shipment, SIV completion, and activation greenlight. The painful failure pattern is declaring progress because many tasks are “in process” while none are complete enough to activate a site. A start-up dashboard should link to CRC regulatory document management, GCP compliance for coordinators, site qualification visits, and investigator site management.
Enrollment milestones require weekly pressure, not monthly surprise. The team should compare actual screening and randomization against forecast, then separate causes: insufficient referrals, strict eligibility, slow prescreening, high screen failures, poor site engagement, patient burden, missing recruitment materials, or competing trials. A site missing enrollment because it has no patients needs a different intervention from a site with patients but slow workflow. Smart teams combine patient recruitment mastery, informed consent best practices, clinical trial volunteer platforms, and patient education resources to diagnose the true bottleneck.
Monitoring milestones protect data quality while the trial is still moving. A monitoring plan should define visit cadence, remote review scope, SDV and SDR priorities, critical data checks, follow-up letter timelines, open issue aging, and escalation thresholds. The study becomes fragile when enrollment accelerates faster than monitoring capacity. CRAs should not discover at month six that consent deviations, AE gaps, and endpoint source issues began in month two. The monitoring rhythm should follow CRA essential monitoring techniques, CRA documentation techniques, GCP compliance for CRAs, and clinical trial auditing readiness.
Data milestones should begin during enrollment, not after last patient last visit. Query aging, missing pages, external lab transfers, coding status, SAE reconciliation, endpoint review, protocol deviation classification, and vendor data uploads should be reviewed throughout the study. Database lock becomes painful when the team treats data cleaning as an end-stage activity. Better teams connect CRF best practices, clinical data management systems, EDC systems, and clinical data manager terminology into the timeline from the start.
Closeout milestones are inspection milestones. Drug accountability, final monitoring, query closure, essential document reconciliation, TMF completeness, site payment closure, archive confirmation, and final safety reconciliation must all be controlled. A rushed closeout creates long-term evidence problems, especially when staff leave and memory disappears. Strong closeout planning uses handling clinical trial audits, research compliance and ethics, PI responsibilities, and clinical trial documentation under GCP.
Which milestone is most likely to derail your clinical trial timeline?
Select the pressure point that creates the most stress in your study operations.
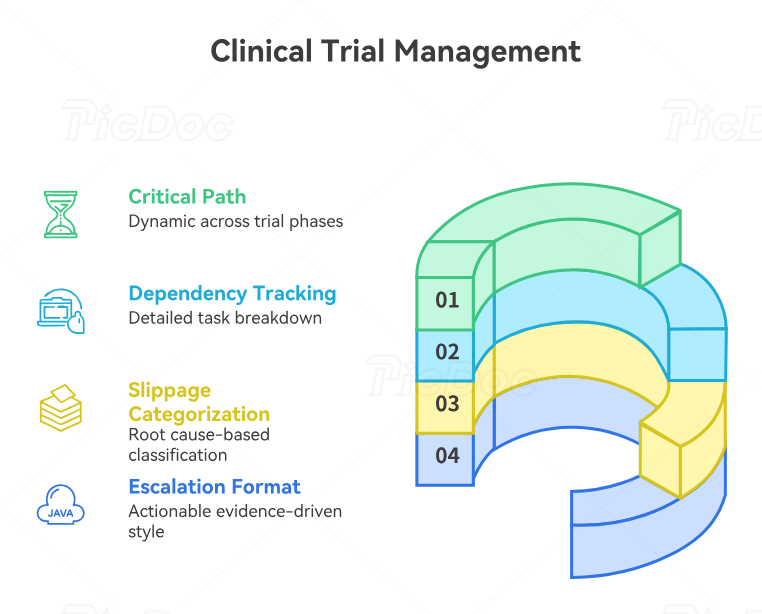
4. Track Critical Path, Dependencies, and Slippage Before the Study Loses Control
The critical path is the chain of tasks that determines the earliest possible completion date. In clinical trials, the critical path often moves. During start-up, it may be contracts, IRB, or drug supply. During recruitment, it may become enrollment velocity. During treatment, it may become monitoring capacity or endpoint completion. Near closeout, it may become query closure, external vendor data, coding, or final document reconciliation. A competent project manager reviews the critical path weekly and connects findings to clinical trial project management terms, risk management practices, resource allocation mastery, and stakeholder communication.
Dependency tracking must be specific. “EDC build” is too broad. Break it into CRF finalization, edit check specifications, UAT, role permissions, randomization integration, lab data integration, training environment, production release, and site access. “Site activation” should break into contract, budget, IRB approval, consent version, essential documents, delegation log, training, SIV, supplies, and greenlight. This level of detail helps teams avoid vague status updates. It also aligns with case report form design, interactive start-up checklists, regulatory document control, and GCP self-assessment tools.
Slippage should be categorized by cause, not blamed on “delay.” A milestone can slip due to decision delay, vendor delay, site capacity, unclear ownership, unrealistic assumptions, protocol complexity, regulatory review, data quality problems, recruitment weakness, supply chain constraints, or unresolved safety questions. Categorization prevents shallow fixes. A recruitment delay does not always need more sites; it may need better prescreening, broader referral networks, fewer site-level workflow barriers, or clearer consent materials. This diagnosis should use clinical trial volunteer registries, informed consent knowledge, CRC responsibilities, and clinical trial protocol management.
The best escalation format is short and evidence-driven: milestone at risk, current variance, root cause, downstream impact, decision needed, owner, due date, and recovery plan. Escalation fails when it sounds emotional or vague. “Site is slow” is weak. “Site 014 has missed document submission by 12 business days, IRB package is blocked, activation forecast moves from May 4 to May 26, and sponsor legal approval is needed today on payment language” is actionable. This style reflects stakeholder communication strategy, vendor management discipline, clinical research PM planning, and clinical trial budget oversight.
5. A Practical Milestone Control System for Sponsors, CROs, CRAs, CRCs, and PMs
Start with one source of truth. The study timeline should include every key milestone, owner, baseline date, current forecast, actual date, status, variance, dependency, risk rating, escalation path, and recovery action. Multiple trackers create multiple realities. Sponsors, CROs, CRAs, CRCs, vendors, and data teams should work from one controlled view. This does not require a complicated system; it requires disciplined updates and honest status. The control system should support clinical trial sponsor roles, clinical trial PM responsibilities, CRA responsibilities, and CRC responsibilities.
Next, create milestone gates. A gate is a formal readiness checkpoint that prevents false progress. For example, a site activation gate should require final CTA, budget, IRB approval, correct consent version, essential documents, delegation log, system access, training, supply confirmation, and SIV completion. A database lock gate should require query closure, coding completion, external data reconciliation, SAE reconciliation, protocol deviation review, PI sign-off, and data management approval. Gates help teams avoid the dangerous habit of counting “almost ready” as ready. They align with clinical trial documentation, protocol deviation management, drug safety reporting, and clinical data management.
Then run milestone meetings around decisions, not updates. Status meetings become wasteful when each function reads from its tracker. A strong meeting focuses on blocked decisions, critical-path movement, milestone variance, risk triggers, recovery plans, and owner accountability. The best question is not “What is the status?” The better question is “What changed since last week that affects the next critical milestone?” This keeps the discussion tied to risk management, resource allocation, effective communication, and clinical trial technology systems.
Finally, create a recovery plan before the timeline breaks. Recovery options may include adding sites, reallocating CRA coverage, increasing remote monitoring, compressing document review cycles, adding recruitment support, prioritizing high-performing sites, accelerating data cleaning, or escalating vendor commitments. Recovery should protect quality. A faster timeline that creates consent errors, data gaps, missed safety reporting, or protocol deviations is a false recovery. Every recovery decision should be reviewed against GCP compliance essentials, adverse event reporting, patient safety oversight, and inspection readiness.
6. FAQs: Clinical Trial Timelines & Milestones Management
-
The most important milestones are protocol finalization, vendor readiness, site selection, regulatory submission, IRB approval, contract execution, site initiation, first site activated, first patient screened, first patient randomized, enrollment completion, last patient last visit, database lock, final analysis, CSR completion, site closeout, and archiving. Each milestone should have an owner, dependency, baseline date, forecast date, and proof artifact. Strong management connects clinical trial project planning, site selection, CRF planning, and clinical trial documentation.
-
Build the timeline from the protocol, schedule of activities, endpoint requirements, country start-up needs, site capacity, vendor dependencies, recruitment assumptions, monitoring plan, data flow, and closeout requirements. Then add dependency logic and risk-based buffers around uncertain work. The strongest timelines use operational evidence rather than optimism. This requires command of clinical trial protocol design, endpoint planning, vendor management, and risk management.
-
Timelines usually slip because dependencies were poorly mapped, site activation was overestimated, enrollment assumptions were too aggressive, vendors delivered late, contracts stalled, data cleaning started too late, or monitoring capacity failed to match study activity. The visible delay is often the final symptom of earlier weak planning. Teams can prevent this by tracking clinical trial resource allocation, patient recruitment, CRA monitoring, and data management systems.
-
Teams should track enrollment by site and by funnel stage: prescreened, screened, screen failed, randomized, withdrawn, and completed. They should also track screen failure reasons, referral source quality, visit burden, consent barriers, competing trials, and coordinator capacity. Enrollment recovery should be specific, not generic. The team may need stronger prescreening, improved site support, better patient education, or additional qualified sites. This should connect CRC recruitment skills, informed consent best practices, volunteer registries, and patient education resources.
-
CRAs help protect timelines by identifying site activation issues, monitoring visit delays, documentation gaps, protocol deviations, query backlogs, consent problems, safety reporting concerns, and repeat site performance issues. A CRA’s monitoring report should show whether the site is on track operationally and whether any issue threatens future milestones. CRA timeline value depends on CRA role clarity, monitoring techniques, GCP compliance, and inspection readiness.
-
A study team can recover by identifying the true critical-path blocker, assigning one accountable owner, compressing review cycles, prioritizing high-performing sites, adding targeted recruitment support, increasing monitoring capacity, improving vendor escalation, and starting data cleaning earlier. Recovery should be measured by milestone impact and quality protection. It should never create shortcuts around consent, safety, data integrity, or protocol compliance. Strong recovery planning uses project management techniques, stakeholder communication, protocol deviation controls, and GCP audit preparation.